What is constipation?
Constipation is the infrequent or difficult passage of stool. It is generally described as having fewer than 3 bowel movements a week, prolonged straining to evacuate stools, incomplete emptying, and/or the passage of hard stools. Causes of constipation include proctologic disorders such as anal fissure, thyroid or parathyroid hormone disease, diabetes, pregnancy, neurologic conditions that affect the muscles of the colon and rectum (Parkinson’s disease, multiple sclerosis, stroke), and weakened pelvic floor muscles. Less commonly are serious conditions such as bowel obstruction from cancer. By far, the most common causes of constipation are lifestyle related including lack of physical activity, poor diet, and low water intake. Constipation can lead to abdominal pain with bloating, colon inflammation (diverticulitis), and proctologic disorders such as hemorrhoids and fissure.
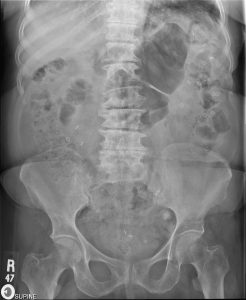
X-Ray motility study in a patient with severe constipation.
How is constipation evaluated?
Dr. Maher Abbas will assess your symptoms and perform a physical examination to determine the type of testing needed. For some patients no testing is needed. Yet for others, 1 or more of the following tests is ordered to assess constipation:
- Blood test for thyroid hormones and calcium level
- Endoscopic examination of the colon and rectum (sigmoidoscopy or colonoscopy [see sections on Sigmoidoscopy and Colonoscopy]
- Anorectal manometry test to evaluate the anal sphincter muscle function [see Manometry]
- Colonic transit study to check for colon function. In this procedure, you swallow a capsule that contains small ring markers which travel through the intestine. XRAY films are obtained 3 and 5 days later to assess how fast these markers travel through the colon
- Dynamic MRI defecography to check for pelvic floor function. During this procedure, contrast gel is inserted into the rectum and in some cases the vagina. MRI pictures are obtained at rest and while you try to defecate to visualize what happens with the internal pelvic organs.
How is constipation treated?
Most patients with constipation are treated medically. Surgery is reserved for severe cases of constipation with a lazy colon or for pelvic floor conditions such as rectocele or rectal prolapse. Medical treatment includes the following:
- Behavioral changes: don’t ignore the urge to pass stool. Avoid sitting on the toilet for prolonged period of time. Lift your feet off the ground and place on a small step [15 to 20 cm high]
- Physical activity: stay as active as possible and try to get regular exercise, at least 30 minutes 4 times a week
- Dietary modifications: include plenty of high-fiber foods in your diet, including beans, vegetables, fruits, whole grain cereals and bran [see section on High Fiber Food]. Gradually increase your fiber intake to avoid bloating and gas. Avoid too much processed food and meat products. Drink at least 8 glasses of water every day
- Fiber supplements: fiber supplements can be added to your diet [see section on Fiber Supplements]
- Laxatives: several laxatives and stimulants can be helpful. If indicated, Dr. Maher Abbas will discuss with you and prescribe [see section on Laxatives]
- Probiotics: some patients can benefits from some types of good bacteria which can promote digestive health
- Enemas and suppositories: in some cases, you may benefit from enemas and rectal irrigation [see sections on How To Do An Enema and Rectal Irrigation]. Several anal suppositories can be helpful including glycerin and Bisacodyl
- Biofeedback training: if a pelvic floor issue is diagnosed, physical therapy in the form of biofeedback training can be helpful [see section on Biofeedback / Kegel Exercises]. You will be referred by Dr. Maher Abbas to the appropriate therapist
Follow-up appointment
An appointment for testing, treatment, or follow-up will be scheduled according to your needs.
Any questions? Contact Dr Maher A. Abbas’ office nurse here.
